I
Hemochromatosis:
How
to
Get
Tested
Where can I get tested for hereditary hemochromatosis? Here is an easy way to get direct testing without a prescription and results sent directly to the patient only. Call Healthcheck USA www.healthcheckusa.com toll free at 1-800-929-2044 for a testing lab near you. Blood testing to check your iron storage status, known as a complete iron profile, which includes, serum iron, TIBC and serum ferritin, is available. If you have a doctor, you may have this testing done by him/her in the office, but remember that the results will then be a part of your medical records, and you may wish to keep that informatio private. Be sure to ask your doctor for these tests by name and obtain and review copies of your test results and keep a home medical file. Genetic Labs Performing DNA Testing for Hereditary Hemochromatosis This is the latest technology in medicine which will quickly and accurately determine if you have the HFE (HH) mutation for hereditary hemochromatosis (HH). This test can help confirm the diagnosis of hereditary hemochromatosis in the presence of elevated transferrin saturation percentage and elevated serum ferritin. In some cases, this test can help the doctor to avoid the traditional (and invasive) liver biopsy for the patient when the ferritin is only slightly elevated (early diagnosis) and no other signs of liver distress are evident such as elevated liver enzymes. Another significant use of the DNA test is screening other family members for their genetic risk once one family member has been identified with the mutation. This is particularly useful in children to identify them at an early age so that the pediatrician can monitor the child throughout childhood for iron storage. AHS advocates newborn screening with the genetic test to have the earliest possible awareness of this mutation being present so that the life of the child may be protected through close monitoring by the pediatrician. Sandra Thomas believes that everyone should have the genetic (DNA) test, whether or not they have a family history of HH or symptoms of HH. Only testing can show you for sure if you, or your family, is at risk for HH and if the HH gene mutation, known as the HFE mutation, is present in your family gene pool.
Sandra Thomas, President/Founder of the American Hemochromatosis Society, discusses iron overload and hemochromatosis with the "Iron King", William Crosby, MD. Dr. Crosby was a pioneer in the field of iron overload/hemochromatosis research and was a good friend to the Thomas family during Sandra's mother's battle with hemochromatosis.
Warning: The doctors on the Board of Directors of The American Hemochromatosis Society state that transferrin saturation percentage greater than 40% and serum ferritin greater than 150ng/mL could indicate clinical iron overload/iron storage in the body and treatment with phlebotomy (bloodletting) should be considered regardless of DNA test results. This means that patients' treatment should not be based on genetic test results alone whether positive or negative. The DNA test is a powerful tool to help us find people at risk; 85-98% of patients with clinical iron overload have the hemochromatosis mutations, however, the most important point to remember is that excess iron needs to be evaluated and treated. William Crosby, MD, (see photo above) the late well known hemochromatosis physician and researcher, declared that if a patient has demonstrated excess iron then they are in danger of organ damage and premature death. Patients should be aggressively (usual rate is weekly or twice weekly depending on the stage of the disease) treated with phlebotomy (bloodletting identical to blood donation) for excess iron! Treatment frequency can be adjusted for individual patients with special circumstances (elderly, other medical problems, etc.) See AHS guidelines
AHS President/Founder, Sandra Thomas, holding a tube of her own blood. Sandra is a "silent carrier" (heterozygote) of the cys282 HFE gene mutation for hereditary hemochromatosis (HH). WARNING: HLA-typing is NOT the same as DNA genetic testing. HLA typing is an outdated form of testing that does not identify the gene mutation for hereditary hemochromatosis. Make sure that you and your doctor are not ordering HLA typing, but rather genetic testing by PCR for the HFE mutation (cys282 and his63) on the short arm of chromosome 6. A few labs also offer testing for the 65C gene mutation, but most labs test only for the cys282 and his63 gene mutations. If you have any questions about DNA testing, please call Sandra Thomas at: 407-829-4488. Other labs offering DNA testing for the HFE gene mutation: GeneTrack (www.hemochromatosisdna.com) Tests adults and children. $156.00 discounted price. Lab Corps/Quest--requires needle in arm and costs $480.00 out of pocket (same test as Gene Track which is only $156.00) Gene Track does not require a doctor's order. In Australia: DNA testing is available at the Queensland Institute of Medical Research at the Royal Brisbane Hospital. They have a web site at: Other Considerations and Thoughts for You: *If you use a doctor for testing (rather than doing it yourself), do not simply ask your doctor to test you for iron overload/hereditaryhemochromatosis, but rather ask for these blood tests by name: serum iron,TIBC (total iron binding capacity), and serum ferritin (blood taken in the doctor's office from your arm not your finger.) Remember hematocrit (hct )and hemoglobin (hgb) are not tests to confirm HH. If you want the fastest and easiest way to find out if you have hemochromatosis, simply call HealthCheckUSA.com and order the tests yourself. You'll have your results in a few days. And, it is completely private. You can get DNA test results from GeneTrack. *Percent of saturation is calculated by dividing the numerical result of the serum iron by the numerical result of the TIBC. A percent of saturationgreater than 40% (>40%) and/or a serum ferritin greater than 150 ng/ml (>150ng/ml) is suggestive of HH and should be further investigated by a qualified physician. *DNA (genetic) testing by a lab which tests for both HFE mutations (cys282 & his63) can help confirm the diagnosis in the presence of high iron levels or determine genetic risk for HH in patients with normal iron levels who may be at high risk of storing iron in the future. Patients who have normal iron levels but who are positive for the HH mutations should be put in a surveillance program by their doctors. If you wish to simplify the process, genetically test yourself using a DNA genetic test kit. Call GeneTrack.com (www.hemochromatosisdna.com) or their toll free number: 1-877-714-6356. *Always get copies of your own lab results and medical records and read them yourself. Keep a master set of medical records in a home medical file; never give out your original master set records, make copies instead, to give to doctors you may visit for additional opinions.. *Always consider getting a second opinion or even multiple, medical opinions, especially if you have an advanced case of HH with serious medical complications. You may have to travel out of town, but it will be worth it. Contact AHS for the names of top experts around the country. *Avoid eating or handling raw seafood, especially if you have liver disease due to HH (or any cause) cooked seafood is fine; do not take vitamin C supplements (natural sources such as orange juice are fine);and do not take iron supplements or vitamins with iron; do not cook food in cast iron cookware. *Do not eat a diet void of iron, it is unpleasant, unhealthy, and you will end up weak! (one patient reported eating nothing but water and cottage cheese the first two weeks after her diagnosis she was so fearful of eating anything with iron in it). Remember our diet motto: “All take heed, you may eat the food that you need, but be willing to bleed!” *Aggressive bloodletting (therapeutic phlebotomy/TP) should be the treatment of choice with 1 unit of blood removed usually once or twice a week, until serum ferritin is less than 20ng/ml (<20) and then maintain it between 20 and 50 for life, then performing 3 to 4 treatments per year for the lifetime of the patient. Treatments should be individualized to each patient, taking into consideration the age, size, weight, and stage of HH of the patient, so that frequency of treatments and amount of blood removed can be adjusted accordingly. *Liver biopsy may be necessary to determine extent of advanced liver disease if liver function tests (LFT’s) are significantly elevated and there are signs of liver distress. Discuss the need for this procedure carefully with your physician. Those with early, asymptomatic HH with normal LFT’s, probably will be able to forego this invasive, and potentially risky procedure. The earlier the diagnosis, the less chance you’ll need a liver biopsy, so early screening is important. If you do have a liver biopsy, request that it be done with “guidance” such as ultrasound or CT and don’t take aspirin type medications a week prior to the procedure. Liver biopsy is used to diagnose, not screen for, primary liver cancer (PLC) . Patients at high risk for PLC should be screened every three to six months with alpha fetoprotein and PIVKA-II blood tests for the rest of their lives. If you refuse to have a liver biopsy, you can still be treated. If your doctor refuses to treat you without a liver biopsy being done first, find another specialist who will. *Warn all family members to be tested and keep a computer file of family members’ results. Don’t forget the elderly and the kids when screening family members. Remember, men, women, and children can get iron overload/HH. *Download a copy of the Annals of Internal Medicine, December 1998 supplement on the “Diagnosis and Management of Hereditary Hemochromatosis” at http://www.acponline.org/journals/annals/01dec98/ mgmthemo.htm and show it to your doctor. *Take an active part in your health care. Ask questions, take notes, research information, keep records, and educate yourself. It’s your life!
Hemochromatosis: Treatment Have you ever donated blood? If you have, then you know exactly what the treatment is for hemochromatosis!
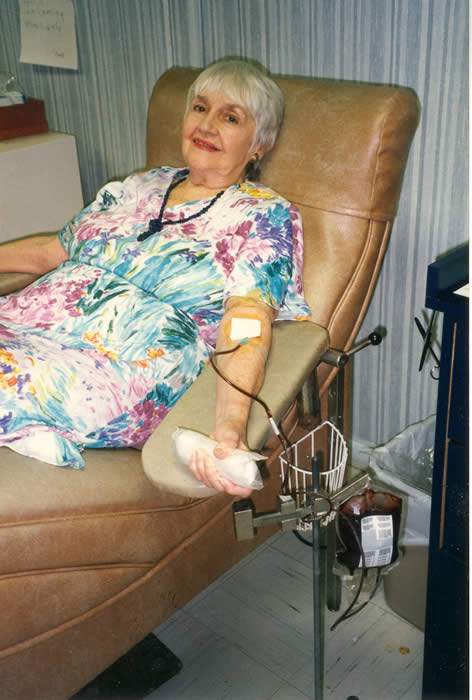
Josephine Bogie Thomas donates blood to control her advanced stage hereditary hemochromatosis. It took 85 treatments to get her "de-ironed" with a total 106 treatments in her lifetime. These phlebotomy treatments done at a local blood bank added another 16 years to her life!
Treatment, also known as therapeutic phebotomy (TP), or "bloodletting" can take place in several locations--a doctor's office, a hospital blood bank, or a community blood bank. Insurance often covers doctor's office and hospital treatments, but not blood banks. If you are paying out of pocket, blood banks would be your best choice since some blood banks will remove the blood for free and use the blood as donor blood. These blood banks are approved by the FDA and have applied for and received a "variance" to use hereditary hemochromatosis (HH) blood as donor blood. Regardless of where you are treated, find a nurse/tech whom you like and who takes the blood in a comfortable fashion. "Bloodletting" as it is sometimes called, is an "art" and you want to find someone who has the "talent" to do it well. The truth is, some people are better at taking blood than others, so when you find that someone "special", you need to find out his/her name and schedule and make sure that your treatment coincide with their hours. Be sure to call the blood bank first, for instance, to make sure that they are there for their regular shift and wait until they are available. This is a handy tip that will make your treatment experience a positive one. Be sure to eat well before and after your treatment, and also drink plenty of fluids before and after treatment. Until you are used to the procedure, take someone with you to drive and give you support, so that you are more relaxed about your experience. If it is your first time, be sure to let the staff know any concerns or fears that you might have. This will help them to be more sensitive to your needs. If you are afraid of needles, you are not alone! Many patients feel this way, but with experience and a supportive staff, they overcome this fear even in the most extreme cases and proceed on with their treatment. If your anxiety is great, let your doctor know. Don't suffer in silence. Your doctor can prescribe a mild sedative that can "take the edge off" of your anxiety and help you to help yourself through your treatment schedule. Most patients want to know how many treatments they will need. That number will depend on what stage of the disease the patient has. If it is an early stage diagnosis, they may only need a few treatments before being "de-ironed". Other patients with more advanced cases, for instance, a ferritin level greater than 1,000, may need dozens of treatments before reducing the iron storage burden to the level it needs to be (a ferritin of 20 is the usual goal, then keep the ferritin between 20 and 50 for the rest of the patient's life). The usual frequency of the treatments are once a week and in advanced cases, sometimes twice a week. Based on various factors, age, health, and weight/size, some patients may be treated less frequently, for instance, every other week, or once a month. In general, though, if the patient has a high ferritin (500 or greater) and is basically in good health otherwise, a minimum of once a week is advised. The weekly treatments will continue until the ferritin reaches 20. At this point, the patient is "de-ironed". The patient can now reduce the treatments to about three to four times a year. This schedule will vary from patient to patient. Some patients need to be treated once a month indefinitely, whereas other patients only need one or two treatments a year. Some of this frequency will depend on the patient's diet and how strict they are with themselves concerning iron intake through their diet. The treatment is usually simple and easy. It should not be a source of great anxiety or discomfort. If it is, then it is time to talk with the doctor, change doctors, change blood banks, or get counseling concerning what is bothering the patient. Treatment is key to saving the patient's life in advanced cases, and to preventing organ damage and premature death in earlier stage cases. Many patients report feeling so much better after each treatment. Some are treated during their lunch break. It is normal to feel tired a few days after the treatment, but remember, each time you give blood, you are reducing the iron stores in your body! Don't give up! Each treatment is bringing you closer to saving your own life!
Sandra Thomas, President, AHS
JAMA (Journal of the American Medical Society), March 19, 2003--Vol. 289, No. 11
|
||||